https://news.sina.com.cn/c/2020-03-17/doc-iimxxstf9803780.shtml
武汉金银潭医院1775名新冠患者研究:O型血相对不易感
2020年03月17日 21:22 澎湃新闻
0
原标题:武汉金银潭医院1775名新冠患者研究:O型血相对不易感
对新冠肺炎患者临床观察表明,老年人、男性更容易感染新冠肺炎并发展为重症。但是,到目前为止,还没有生物标志物可以预测个体对COVID-19的敏感性。南方科技大学、上海交大、武汉中南医院、武汉金银潭医院等8家单位的最新研究显示:A、B、O、AB血型与新冠肺炎易感性存在关联。这也是该领域的首份研究。
具体来说,O型血对新冠肺炎相对不易感,风险较低;A型血对新冠肺炎相对易感,风险也较高。该研究提示:
(1)A型血可能需要特别加强个人保护以减少感染机会;
(2)新冠病毒感染的A型血患者可能需要接受更多的监护和治疗;
(3)作为新冠病毒治疗的常规部分,在患者和医务人员中引入ABO血型可能会帮助评估人们的风险暴露水平。
以上研究来自论文“Relationship between the ABO Blood Group and the COVID-19 Susceptibility”。该论文于当地时间3月17日刊发在预印本平台medRxiv,尚未经同行评议。
该研究的样本来自武汉和深圳的三家三甲医院,分别是:武汉市金银潭医院的1775例COVID-19患者,其中206例死亡;武汉大学人民医院的113名患者;深圳市第三人民医院的285名患者。研究人员主要检测这些患者的ABO血型,新冠肺炎的感染发生情况以及死亡情况。统计分析采用的方法是单因素方差分析 (one-way ANOVA)和双尾(2-tailed)卡方检验。研究还设置了随机效应模型(REM),对不同医院的数据进行Meta分析。
研究显示,在武汉市3694名正常人中, A、B、AB和O型血的占比分别为32.16%、24.90%、9.10%和33.84%。而在武汉市金银潭医院的1775名COVID-19患者中,A、B、AB和O的占比37.75%,26.42%,10.03%和25.80%。
值得注意的是,COVID-19患者中血型A比例和O的比例分别显著高于和低于正常人比例(P <0.001)。
武汉大学人民医院和深圳市第三人民医院这两家三甲医院的398名患者也观察到了相似的ABO分布模式。
分析结果显示,与O、B、AB血型相比,A血型的COVID-19感染风险显著升高(OR为1.20;95%置信区间CI为1.02-1.43,P=0.02)。与A、B、AB血型相比,O型血型的传染病风险显著降低(OR为0.67;95%CI为0.60-0.75,P <0.001)。
也就是说,与非A血型相比,具有A血型的人获得COVID-19的风险明显更高,而与O血型相比,O血型的感染风险显著降低。
此前也有一些研究显示,一些病毒感染的易感性与ABO血型有关。例如,诺沃克病毒和乙型肝炎具有明确的血型易感性。而据此前报道,O型血的个体感染SARS冠状病毒的可能性也较小。
该论文有8家科研机构,分别是:南方科技大学、深圳市第三人民医院(南方科技大学第二附属医院)、武汉市金银潭医院、武汉大学人民医院、中国医学科学院阜外医院、华东师范大学、武汉大学中南医院、上海交通大学。
通讯作者为南方科技大学医学院首任院长、讲席教授邢明照;南方科技大学医学院科研办公室主任、讲席教授王鹏;上海交通大学生命科学技术学院研究员杨广宇;武汉大学中南医院院长、雷神山医院院长王行环等。
附:数据分析部分
武汉市3694名正常人的ABO血型分别显示A、B、AB和O型血型的百分比分布分别为32.16%、24.90%、9.10%和33.84%,而武汉市金银潭医院的1775名COVID-19患者显示A、B、AB和O型血型的ABO分布分别为37.75%、26.42%、10.03%和25.80%。
COVID-19患者中A型血的比例显著高于正常人群,前者为37.75%,后者为32.16%(P <0.001)。COVID-19患者的O型血比例显著低于正常人群,前者为25.80%,后者为33.84%(P <0.001)。
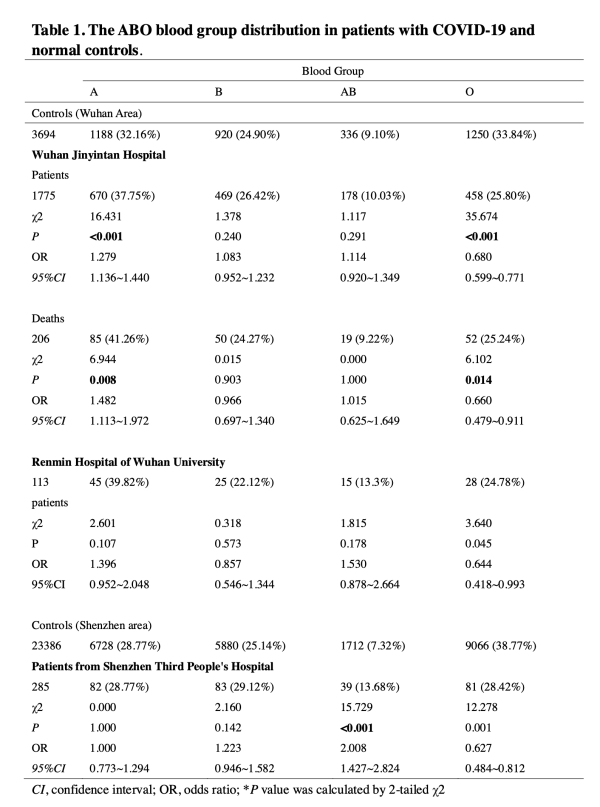
在死亡患者中观察到高危血型A和低危血型O的分布模式也与之相似。具体而言,在206例死亡患者中,A、B、AB和O血型的比例分别为41.26%、24.27%、9.22%和25.24%。与非O型血组相比,O型血死亡风险更低,OR为0.660(95%CI 0.479-0.911,P=0.014)。相反,与非A组相比,A组的死亡风险更高,OR为1.482(95%CI 1.113-1.972,P=0.008)。
接下来,研究团队检查了武汉市另一医院武汉大学人民医院的113例COVID-19患者,发现了ABO血型感染的相似风险分布趋势。具体而言,与非O型血组相比,O型血组与感染风险显著降低,OR为0.644(95%CI 0.418-0.993,P=0.045)。与非A血型相比,A血型的相对危险度更高(OR=1.396; 95%CI 0.952-2.048),比武汉市金银潭医院的患者还要高,尽管由于样本量相对较小,该组相关性没有统计学意义。
深圳23368名正常人的ABO血型分别显示A、B、AB和O血型的百分比分布分别为28.77%、25.14%、7.32%和38.77%。对深圳的285例COVID-19患者的分析显示,A、B、AB和O血型的比例分别为28.77%、29.12%、13.68%和28.42%。
同样,O型血的感染风险显着降低(OR为0.627; 95%CI为0.484-0.812)。此外,研究发现AB血型的感染风险增加(OR为2.008; 95%CI为1.427-2.824)。另外,这285名患者的平均年龄为45.1±18.6岁,其中包括147名男性和138名女性。研究发现不同ABO组的患者年龄无显着差异(F = 0.135; P = 0.939)。
通过随机效应模型显示了来自三家医院的汇总数据对ABO血型的COVID-19风险的OR估计值。结果再次表明,与非A型血型相比,A型血型与COVID-19的风险显著升高(OR为1.21; 95%CI 1.02-1.43,P = 0.027)。与非O型血型相比,感染风险显著降低(OR,0.67; 95%CI 0.60-0.75,P <0.001)血型。与其他ABO血型相比,AB血型(OR,1.48,95%CI 0.97-2.24)和B血型(OR,1.09,95%CI 0.98-1.22)似乎也具有更高的感染风险。不过以上相关性没有达到统计学意义。
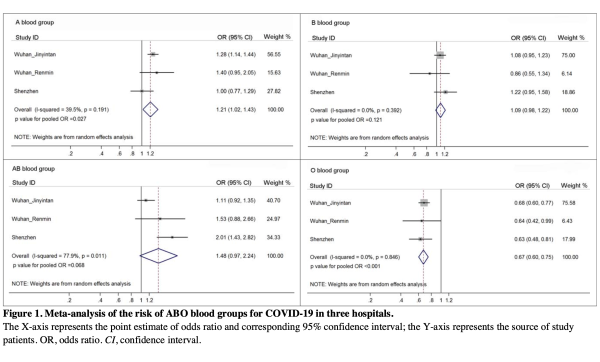
接下来,研究团队调查了年龄和性别这两个危险因素是否会影响COVID-19患者中ABO血型的分布。已知ABO血型分布没有性别和年龄偏向。例如,通过分析超过9万名正常人的血型,可以看出不同年龄段和性别之间的A、B、AB和O血型百分比基本相同。
因此,研究者以武汉地区3694名正常人的ABO血型分布作为对照,以与不同年龄组和性别组进行比较。将武汉市金银潭医院和武汉人民医院的所有患者合并在一起(共1888名患者),并分为三个年龄组(40岁以下,41-59岁,60岁以上),ABO血型分布在各年龄组之间没有变化。同样,当分别考虑COVID-19患者的男女时,ABO血型分布也没有太大变化。
讨论
这项研究发现ABO血型对新冠病毒感染表现出不同的关联风险。具体而言,血型A与风险增加有相关性,而血型O与风险降低有相关性,因此证明ABO血型是COVID-19敏感性差异的生物标志物。
这些发现与先前研究中发现的ABO血型相似的其他冠状病毒感染风险模式一致。比如,此前有研究显示香港的SARS-CoV感染易感性与ABO血型有关。
研究者还发现,与非O型血型医院工作人员相比,O型血型医院工作人员被感染的机会更低。此前有发现抗A抗体特异性抑制SARS-CoV S蛋白表达细胞与ACE2表达细胞系的粘附。鉴于SARS-CoV和SARS-CoV-2之间的核酸序列相似性和受体血管紧张素转换酶2(ACE2)结合相似性,O型血敏感性较低,而A型血对COVID-19的敏感性较高,这与血液中天然抗血型抗体,特别是抗A抗体的存在有关。
研究同时提到,这个假设将需要直接研究来证明。ABO血型对COVID-19的易感性可能还存在其他机制,需要进一步研究加以阐明。
点击进入专题:
聚焦新型冠状病毒肺炎疫情
责任编辑:杨杰
关键字 : ABO血型AB血型新冠肺炎武汉湖北
我要反馈
Study of 1,775 New Crown Patients at Wuhan Jinyintan Hospital: Type O blood is relatively less susceptible
March 17, 2020 21:22 Surging News
0
Original Title: Study of 1,775 New Crown Patients at Wuhan Jinyintan Hospital: Type O blood is relatively less susceptible
Clinical observations of patients with new coronary pneumonia have shown that older people and men are more likely to be infected with new coronary pneumonia and develop severe illness. However, to date, there are no biomarkers that can predict an individual's sensitivity to COVID-19. The latest research from 8 units including Southern University of Science and Technology, Shanghai Jiaotong University, Wuhan Zhongnan Hospital, Wuhan Jinyintan Hospital, etc. showed that blood types of A, B, O, and AB are associated with susceptibility to new coronary pneumonia. This is also the first study in this field.
Specifically, type O blood is relatively less susceptible to new coronary pneumonia and has a lower risk; type A blood is relatively susceptible to new coronary pneumonia and has a higher risk. The study suggests:
(1) Type A blood may require special personal protection to reduce the chance of infection;
(2) Patients with blood type A who are infected with neocoronavirus may require more monitoring and treatment;
(3) As a routine part of neocoronavirus treatment, the introduction of ABO blood types in patients and medical staff may help assess people's level of risk exposure.
The above research is from the paper "Relationship between the ABO Blood Group and the COVID-19 Susceptibility". The paper was published on the preprinted platform medRxiv on March 17, local time, and has not yet been peer reviewed.
The samples from the study were from three top three hospitals in Wuhan and Shenzhen, respectively: 1775 COVID-19 patients in Wuhan Jinyintan Hospital, of which 206 died; 113 patients in Wuhan University People's Hospital; and 285 in Shenzhen Third People's Hospital. Patients. The researchers mainly tested the ABO blood group, the incidence of neocoronary pneumonia, and the deaths in these patients. The methods used for statistical analysis were one-way ANOVA and 2-tailed chi-square test. The study also set up a random effects model (REM) to perform a meta-analysis of data from different hospitals.
Studies show that among 3694 normal people in Wuhan, the proportions of A, B, AB and O blood types were 32.16%, 24.90%, 9.10%, and 33.84%. Among the 1,775 COVID-19 patients at Wuhan Jinyintan Hospital, A, B, AB and O accounted for 37.75%, 26.42%, 10.03% and 25.80%.
It is worth noting that the proportion of blood group A and O in patients with COVID-19 was significantly higher and lower than that of normal people (P <0.001).
Wuhan University People's Hospital and Shenzhen Third People's Hospital, two tertiary hospitals, also observed similar ABO distribution patterns.
The analysis results showed that compared with O, B, and AB blood types, the risk of COVID-19 infection in blood group A was significantly increased (OR was 1.20; 95% confidence interval CI was 1.02-1.43, P = 0.02). Compared with A, B, AB blood types, the risk of infectious diseases of blood type O was significantly reduced (OR was 0.67; 95% CI was 0.60-0.75, P <0.001).
That is, compared with non-A blood group, people with blood group A have a significantly higher risk of acquiring COVID-19, and compared with blood group O, the risk of infection with blood group O is significantly reduced.
Previous studies have shown that the susceptibility of some viral infections is related to the ABO blood group. For example, Norwalk virus and hepatitis B have a clear blood group susceptibility. According to previous reports, individuals with blood type O are less likely to contract SARS coronavirus.
There are 8 scientific research institutions in this thesis: Southern University of Science and Technology, Shenzhen Third People ’s Hospital (Second Affiliated Hospital of Southern University of Science and Technology), Wuhan Jinyintan Hospital, Wuhan University People ’s Hospital, Chinese Academy of Medical Sciences Fuwai Hospital, East China Normal University University, Wuhan University Zhongnan Hospital, Shanghai Jiaotong University.
Corresponding author is Xing Mingzhao, the first dean and chair professor of the School of Medicine, Southern University of Science and Technology; Wang Peng, director and chair professor of the Scientific Research Office of the School of Medicine, Southern University of Science and Technology; , Wang Xinghuan, director of Thunder Mountain Hospital.
Attachment: data analysis part
The ABO blood types of 3694 normal people in Wuhan showed 32.16%, 24.90%, 9.10%, and 33.84% blood type distributions, respectively, and 1775 COVID-19 patients from Wuhan Jinyintan Hospital showed The ABO distributions of A, B, AB, and O blood types were 37.75%, 26.42%, 10.03%, and 25.80%.
The proportion of COVID-19 patients with type A blood was significantly higher than the normal population, the former was 37.75%, and the latter was 32.16% (P <0.001). The proportion of patients with COVID-19 with type O blood was significantly lower than the normal population, with the former being 25.80% and the latter being 33.84% (P <0.001).

Zh
The distribution pattern of high-risk blood group A and low-risk blood group O was also observed in dead patients. Specifically, among the 206 deaths, the proportions of A, B, AB, and O blood types were 41.26%, 24.27%, 9.22%, and 25.24%, respectively. Compared with the non-O blood group, the risk of O blood death was lower, with an OR of 0.660 (95% CI 0.479-0.911, P = 0.014). In contrast, compared with the non-A group, the risk of death was higher in the A group, with an OR of 1.482 (95% CI 1.113-1.972, P = 0.008).
Next, the research team examined 113 COVID-19 patients from Wuhan University People's Hospital, another hospital in Wuhan, and found a similar risk distribution trend for ABO blood group infections. Specifically, compared with the non-O blood group, the O blood group had a significantly lower risk of infection, with an OR of 0.644 (95% CI 0.418-0.993, P = 0.045). Compared with non-A blood group, the relative risk of A blood group is higher (OR = 1.396; 95% CI 0.952-2.048), which is higher than that of patients at Wuhan Jinyintan Hospital, although the group is related because of the relatively small sample size. Sex is not statistically significant.
The ABO blood types of 23,368 normal people in Shenzhen showed that the percentage distributions of A, B, AB and O blood types were 28.77%, 25.14%, 7.32% and 38.77%, respectively. Analysis of 285 COVID-19 patients in Shenzhen showed that the proportions of A, B, AB, and O blood types were 28.77%, 29.12%, 13.68%, and 28.42%, respectively.
Similarly, the risk of infection with blood type O was significantly reduced (OR 0.627; 95% CI 0.484-0.812). In addition, the study found an increased risk of infection with the AB blood group (OR: 2.008; 95% CI: 1.427-2.824). In addition, the average age of these 285 patients was 45.1 ± 18.6 years, including 147 men and 138 women. The study found no significant differences in age among patients in different ABO groups (F = 0.135; P = 0.939).
Randomized effect models show the OR estimates of the COVID-19 risk of the ABO blood group for pooled data from three hospitals. The results again showed that compared with non-A blood types, the risk of blood type A and COVID-19 was significantly increased (OR 1.21; 95% CI 1.02-1.43, P = 0.027). Compared with non-O blood type, the risk of infection was significantly reduced (OR, 0.67; 95% CI 0.60-0.75, P <0.001) blood type. Compared with other ABO blood types, blood group AB (OR, 1.48, 95% CI 0.97-2.24) and blood group B (OR, 1.09, 95% CI 0.98-1.22) also seem to have a higher risk of infection. However, the above correlation did not reach statistical significance.

Zh
Next, the research team investigated whether two risk factors, age and sex, could affect the distribution of ABO blood types in patients with COVID-19. It is known that the distribution of ABO blood types is not gender and age biased. For example, by analyzing the blood types of more than 90,000 normal people, it can be seen that the percentages of A, B, AB, and O blood groups are basically the same between different age groups and genders.
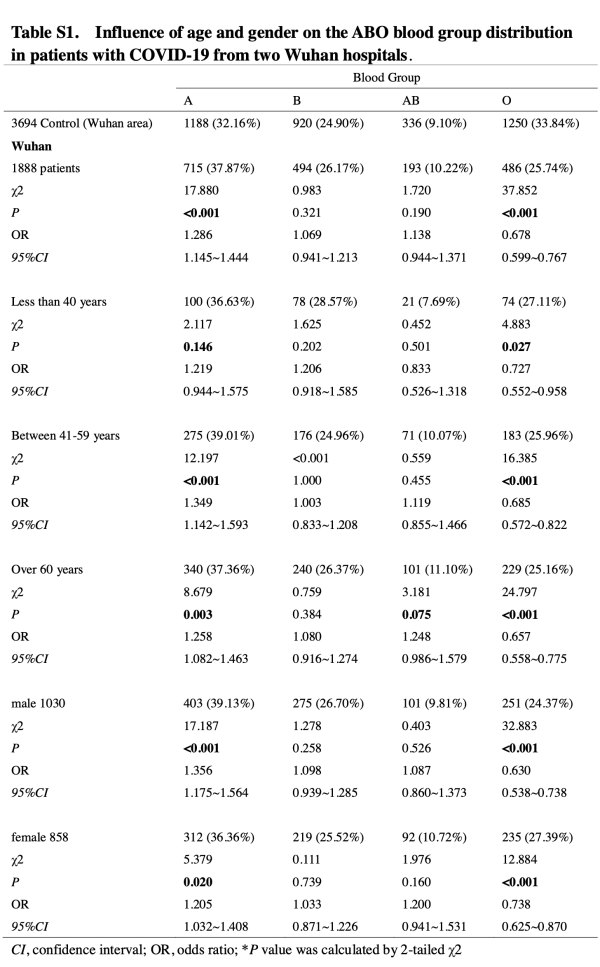
Therefore, the researchers used the ABO blood group distribution of 3694 normal people in Wuhan as a control to compare with different age groups and gender groups. All patients from Wuhan Jinyintan Hospital and Wuhan People's Hospital were merged together (1888 patients in total) and divided into three age groups (under 40 years old, 41-59 years old, and over 60 years old), and the ABO blood type was distributed at each age No change between groups. Similarly, when men and women with COVID-19 were considered separately, the distribution of ABO blood types did not change much.

Zh
Discussion
This study found that the ABO blood group showed different associated risks for neocoronavirus infection. Specifically, blood group A is associated with increased risk, while blood group O is associated with decreased risk, thus proving that the ABO blood group is a biomarker of COVID-19 sensitivity difference.
These findings are consistent with other coronavirus infection risk patterns similar to ABO blood types found in previous studies. For example, previous studies have shown that the susceptibility of SARS-CoV infection in Hong Kong is related to the ABO blood group.
Researchers also found that hospital staff of blood group O were less likely to be infected than those of hospitals of non blood type O. Previously, anti-A antibodies were found to specifically inhibit the adhesion of SARS-CoV S protein-expressing cells to ACE2-expressing cell lines. In view of the similarity of the nucleic acid sequence between SARS-CoV and SARS-CoV-2 and the binding similarity of the receptor angiotensin-converting enzyme 2 (ACE2), the sensitivity of type O blood is low, while type A blood is less Higher sensitivity, which is related to the presence of natural anti-blood antibodies, especially anti-A antibodies, in the blood.
The research also mentions that this hypothesis will require direct research to prove. There may be other mechanisms for the susceptibility of ABO blood group to COVID-19, which needs further research to clarify.
Click to enter the topic:
Spotlight on new coronavirus pneumonia
Editor-in-chief: Yang Jie
Key words: ABO blood group AB blood group new coronary pneumonia Wuhan Hubei
武汉金银潭医院1775名新冠患者研究:O型血相对不易感
2020年03月17日 21:22 澎湃新闻
0
原标题:武汉金银潭医院1775名新冠患者研究:O型血相对不易感
对新冠肺炎患者临床观察表明,老年人、男性更容易感染新冠肺炎并发展为重症。但是,到目前为止,还没有生物标志物可以预测个体对COVID-19的敏感性。南方科技大学、上海交大、武汉中南医院、武汉金银潭医院等8家单位的最新研究显示:A、B、O、AB血型与新冠肺炎易感性存在关联。这也是该领域的首份研究。
具体来说,O型血对新冠肺炎相对不易感,风险较低;A型血对新冠肺炎相对易感,风险也较高。该研究提示:
(1)A型血可能需要特别加强个人保护以减少感染机会;
(2)新冠病毒感染的A型血患者可能需要接受更多的监护和治疗;
(3)作为新冠病毒治疗的常规部分,在患者和医务人员中引入ABO血型可能会帮助评估人们的风险暴露水平。
以上研究来自论文“Relationship between the ABO Blood Group and the COVID-19 Susceptibility”。该论文于当地时间3月17日刊发在预印本平台medRxiv,尚未经同行评议。
该研究的样本来自武汉和深圳的三家三甲医院,分别是:武汉市金银潭医院的1775例COVID-19患者,其中206例死亡;武汉大学人民医院的113名患者;深圳市第三人民医院的285名患者。研究人员主要检测这些患者的ABO血型,新冠肺炎的感染发生情况以及死亡情况。统计分析采用的方法是单因素方差分析 (one-way ANOVA)和双尾(2-tailed)卡方检验。研究还设置了随机效应模型(REM),对不同医院的数据进行Meta分析。
研究显示,在武汉市3694名正常人中, A、B、AB和O型血的占比分别为32.16%、24.90%、9.10%和33.84%。而在武汉市金银潭医院的1775名COVID-19患者中,A、B、AB和O的占比37.75%,26.42%,10.03%和25.80%。
值得注意的是,COVID-19患者中血型A比例和O的比例分别显著高于和低于正常人比例(P <0.001)。
武汉大学人民医院和深圳市第三人民医院这两家三甲医院的398名患者也观察到了相似的ABO分布模式。
分析结果显示,与O、B、AB血型相比,A血型的COVID-19感染风险显著升高(OR为1.20;95%置信区间CI为1.02-1.43,P=0.02)。与A、B、AB血型相比,O型血型的传染病风险显著降低(OR为0.67;95%CI为0.60-0.75,P <0.001)。
也就是说,与非A血型相比,具有A血型的人获得COVID-19的风险明显更高,而与O血型相比,O血型的感染风险显著降低。
此前也有一些研究显示,一些病毒感染的易感性与ABO血型有关。例如,诺沃克病毒和乙型肝炎具有明确的血型易感性。而据此前报道,O型血的个体感染SARS冠状病毒的可能性也较小。
该论文有8家科研机构,分别是:南方科技大学、深圳市第三人民医院(南方科技大学第二附属医院)、武汉市金银潭医院、武汉大学人民医院、中国医学科学院阜外医院、华东师范大学、武汉大学中南医院、上海交通大学。
通讯作者为南方科技大学医学院首任院长、讲席教授邢明照;南方科技大学医学院科研办公室主任、讲席教授王鹏;上海交通大学生命科学技术学院研究员杨广宇;武汉大学中南医院院长、雷神山医院院长王行环等。
附:数据分析部分
武汉市3694名正常人的ABO血型分别显示A、B、AB和O型血型的百分比分布分别为32.16%、24.90%、9.10%和33.84%,而武汉市金银潭医院的1775名COVID-19患者显示A、B、AB和O型血型的ABO分布分别为37.75%、26.42%、10.03%和25.80%。
COVID-19患者中A型血的比例显著高于正常人群,前者为37.75%,后者为32.16%(P <0.001)。COVID-19患者的O型血比例显著低于正常人群,前者为25.80%,后者为33.84%(P <0.001)。

在死亡患者中观察到高危血型A和低危血型O的分布模式也与之相似。具体而言,在206例死亡患者中,A、B、AB和O血型的比例分别为41.26%、24.27%、9.22%和25.24%。与非O型血组相比,O型血死亡风险更低,OR为0.660(95%CI 0.479-0.911,P=0.014)。相反,与非A组相比,A组的死亡风险更高,OR为1.482(95%CI 1.113-1.972,P=0.008)。
接下来,研究团队检查了武汉市另一医院武汉大学人民医院的113例COVID-19患者,发现了ABO血型感染的相似风险分布趋势。具体而言,与非O型血组相比,O型血组与感染风险显著降低,OR为0.644(95%CI 0.418-0.993,P=0.045)。与非A血型相比,A血型的相对危险度更高(OR=1.396; 95%CI 0.952-2.048),比武汉市金银潭医院的患者还要高,尽管由于样本量相对较小,该组相关性没有统计学意义。
深圳23368名正常人的ABO血型分别显示A、B、AB和O血型的百分比分布分别为28.77%、25.14%、7.32%和38.77%。对深圳的285例COVID-19患者的分析显示,A、B、AB和O血型的比例分别为28.77%、29.12%、13.68%和28.42%。
同样,O型血的感染风险显着降低(OR为0.627; 95%CI为0.484-0.812)。此外,研究发现AB血型的感染风险增加(OR为2.008; 95%CI为1.427-2.824)。另外,这285名患者的平均年龄为45.1±18.6岁,其中包括147名男性和138名女性。研究发现不同ABO组的患者年龄无显着差异(F = 0.135; P = 0.939)。
通过随机效应模型显示了来自三家医院的汇总数据对ABO血型的COVID-19风险的OR估计值。结果再次表明,与非A型血型相比,A型血型与COVID-19的风险显著升高(OR为1.21; 95%CI 1.02-1.43,P = 0.027)。与非O型血型相比,感染风险显著降低(OR,0.67; 95%CI 0.60-0.75,P <0.001)血型。与其他ABO血型相比,AB血型(OR,1.48,95%CI 0.97-2.24)和B血型(OR,1.09,95%CI 0.98-1.22)似乎也具有更高的感染风险。不过以上相关性没有达到统计学意义。

接下来,研究团队调查了年龄和性别这两个危险因素是否会影响COVID-19患者中ABO血型的分布。已知ABO血型分布没有性别和年龄偏向。例如,通过分析超过9万名正常人的血型,可以看出不同年龄段和性别之间的A、B、AB和O血型百分比基本相同。
因此,研究者以武汉地区3694名正常人的ABO血型分布作为对照,以与不同年龄组和性别组进行比较。将武汉市金银潭医院和武汉人民医院的所有患者合并在一起(共1888名患者),并分为三个年龄组(40岁以下,41-59岁,60岁以上),ABO血型分布在各年龄组之间没有变化。同样,当分别考虑COVID-19患者的男女时,ABO血型分布也没有太大变化。

讨论
这项研究发现ABO血型对新冠病毒感染表现出不同的关联风险。具体而言,血型A与风险增加有相关性,而血型O与风险降低有相关性,因此证明ABO血型是COVID-19敏感性差异的生物标志物。
这些发现与先前研究中发现的ABO血型相似的其他冠状病毒感染风险模式一致。比如,此前有研究显示香港的SARS-CoV感染易感性与ABO血型有关。
研究者还发现,与非O型血型医院工作人员相比,O型血型医院工作人员被感染的机会更低。此前有发现抗A抗体特异性抑制SARS-CoV S蛋白表达细胞与ACE2表达细胞系的粘附。鉴于SARS-CoV和SARS-CoV-2之间的核酸序列相似性和受体血管紧张素转换酶2(ACE2)结合相似性,O型血敏感性较低,而A型血对COVID-19的敏感性较高,这与血液中天然抗血型抗体,特别是抗A抗体的存在有关。
研究同时提到,这个假设将需要直接研究来证明。ABO血型对COVID-19的易感性可能还存在其他机制,需要进一步研究加以阐明。
点击进入专题:
聚焦新型冠状病毒肺炎疫情
责任编辑:杨杰
关键字 : ABO血型AB血型新冠肺炎武汉湖北
我要反馈
Study of 1,775 New Crown Patients at Wuhan Jinyintan Hospital: Type O blood is relatively less susceptible
March 17, 2020 21:22 Surging News
0
Original Title: Study of 1,775 New Crown Patients at Wuhan Jinyintan Hospital: Type O blood is relatively less susceptible
Clinical observations of patients with new coronary pneumonia have shown that older people and men are more likely to be infected with new coronary pneumonia and develop severe illness. However, to date, there are no biomarkers that can predict an individual's sensitivity to COVID-19. The latest research from 8 units including Southern University of Science and Technology, Shanghai Jiaotong University, Wuhan Zhongnan Hospital, Wuhan Jinyintan Hospital, etc. showed that blood types of A, B, O, and AB are associated with susceptibility to new coronary pneumonia. This is also the first study in this field.
Specifically, type O blood is relatively less susceptible to new coronary pneumonia and has a lower risk; type A blood is relatively susceptible to new coronary pneumonia and has a higher risk. The study suggests:
(1) Type A blood may require special personal protection to reduce the chance of infection;
(2) Patients with blood type A who are infected with neocoronavirus may require more monitoring and treatment;
(3) As a routine part of neocoronavirus treatment, the introduction of ABO blood types in patients and medical staff may help assess people's level of risk exposure.
The above research is from the paper "Relationship between the ABO Blood Group and the COVID-19 Susceptibility". The paper was published on the preprinted platform medRxiv on March 17, local time, and has not yet been peer reviewed.
The samples from the study were from three top three hospitals in Wuhan and Shenzhen, respectively: 1775 COVID-19 patients in Wuhan Jinyintan Hospital, of which 206 died; 113 patients in Wuhan University People's Hospital; and 285 in Shenzhen Third People's Hospital. Patients. The researchers mainly tested the ABO blood group, the incidence of neocoronary pneumonia, and the deaths in these patients. The methods used for statistical analysis were one-way ANOVA and 2-tailed chi-square test. The study also set up a random effects model (REM) to perform a meta-analysis of data from different hospitals.
Studies show that among 3694 normal people in Wuhan, the proportions of A, B, AB and O blood types were 32.16%, 24.90%, 9.10%, and 33.84%. Among the 1,775 COVID-19 patients at Wuhan Jinyintan Hospital, A, B, AB and O accounted for 37.75%, 26.42%, 10.03% and 25.80%.
It is worth noting that the proportion of blood group A and O in patients with COVID-19 was significantly higher and lower than that of normal people (P <0.001).
Wuhan University People's Hospital and Shenzhen Third People's Hospital, two tertiary hospitals, also observed similar ABO distribution patterns.
The analysis results showed that compared with O, B, and AB blood types, the risk of COVID-19 infection in blood group A was significantly increased (OR was 1.20; 95% confidence interval CI was 1.02-1.43, P = 0.02). Compared with A, B, AB blood types, the risk of infectious diseases of blood type O was significantly reduced (OR was 0.67; 95% CI was 0.60-0.75, P <0.001).
That is, compared with non-A blood group, people with blood group A have a significantly higher risk of acquiring COVID-19, and compared with blood group O, the risk of infection with blood group O is significantly reduced.
Previous studies have shown that the susceptibility of some viral infections is related to the ABO blood group. For example, Norwalk virus and hepatitis B have a clear blood group susceptibility. According to previous reports, individuals with blood type O are less likely to contract SARS coronavirus.
There are 8 scientific research institutions in this thesis: Southern University of Science and Technology, Shenzhen Third People ’s Hospital (Second Affiliated Hospital of Southern University of Science and Technology), Wuhan Jinyintan Hospital, Wuhan University People ’s Hospital, Chinese Academy of Medical Sciences Fuwai Hospital, East China Normal University University, Wuhan University Zhongnan Hospital, Shanghai Jiaotong University.
Corresponding author is Xing Mingzhao, the first dean and chair professor of the School of Medicine, Southern University of Science and Technology; Wang Peng, director and chair professor of the Scientific Research Office of the School of Medicine, Southern University of Science and Technology; , Wang Xinghuan, director of Thunder Mountain Hospital.
Attachment: data analysis part
The ABO blood types of 3694 normal people in Wuhan showed 32.16%, 24.90%, 9.10%, and 33.84% blood type distributions, respectively, and 1775 COVID-19 patients from Wuhan Jinyintan Hospital showed The ABO distributions of A, B, AB, and O blood types were 37.75%, 26.42%, 10.03%, and 25.80%.
The proportion of COVID-19 patients with type A blood was significantly higher than the normal population, the former was 37.75%, and the latter was 32.16% (P <0.001). The proportion of patients with COVID-19 with type O blood was significantly lower than the normal population, with the former being 25.80% and the latter being 33.84% (P <0.001).

Zh
The distribution pattern of high-risk blood group A and low-risk blood group O was also observed in dead patients. Specifically, among the 206 deaths, the proportions of A, B, AB, and O blood types were 41.26%, 24.27%, 9.22%, and 25.24%, respectively. Compared with the non-O blood group, the risk of O blood death was lower, with an OR of 0.660 (95% CI 0.479-0.911, P = 0.014). In contrast, compared with the non-A group, the risk of death was higher in the A group, with an OR of 1.482 (95% CI 1.113-1.972, P = 0.008).
Next, the research team examined 113 COVID-19 patients from Wuhan University People's Hospital, another hospital in Wuhan, and found a similar risk distribution trend for ABO blood group infections. Specifically, compared with the non-O blood group, the O blood group had a significantly lower risk of infection, with an OR of 0.644 (95% CI 0.418-0.993, P = 0.045). Compared with non-A blood group, the relative risk of A blood group is higher (OR = 1.396; 95% CI 0.952-2.048), which is higher than that of patients at Wuhan Jinyintan Hospital, although the group is related because of the relatively small sample size. Sex is not statistically significant.
The ABO blood types of 23,368 normal people in Shenzhen showed that the percentage distributions of A, B, AB and O blood types were 28.77%, 25.14%, 7.32% and 38.77%, respectively. Analysis of 285 COVID-19 patients in Shenzhen showed that the proportions of A, B, AB, and O blood types were 28.77%, 29.12%, 13.68%, and 28.42%, respectively.
Similarly, the risk of infection with blood type O was significantly reduced (OR 0.627; 95% CI 0.484-0.812). In addition, the study found an increased risk of infection with the AB blood group (OR: 2.008; 95% CI: 1.427-2.824). In addition, the average age of these 285 patients was 45.1 ± 18.6 years, including 147 men and 138 women. The study found no significant differences in age among patients in different ABO groups (F = 0.135; P = 0.939).
Randomized effect models show the OR estimates of the COVID-19 risk of the ABO blood group for pooled data from three hospitals. The results again showed that compared with non-A blood types, the risk of blood type A and COVID-19 was significantly increased (OR 1.21; 95% CI 1.02-1.43, P = 0.027). Compared with non-O blood type, the risk of infection was significantly reduced (OR, 0.67; 95% CI 0.60-0.75, P <0.001) blood type. Compared with other ABO blood types, blood group AB (OR, 1.48, 95% CI 0.97-2.24) and blood group B (OR, 1.09, 95% CI 0.98-1.22) also seem to have a higher risk of infection. However, the above correlation did not reach statistical significance.

Zh
Next, the research team investigated whether two risk factors, age and sex, could affect the distribution of ABO blood types in patients with COVID-19. It is known that the distribution of ABO blood types is not gender and age biased. For example, by analyzing the blood types of more than 90,000 normal people, it can be seen that the percentages of A, B, AB, and O blood groups are basically the same between different age groups and genders.
Therefore, the researchers used the ABO blood group distribution of 3694 normal people in Wuhan as a control to compare with different age groups and gender groups. All patients from Wuhan Jinyintan Hospital and Wuhan People's Hospital were merged together (1888 patients in total) and divided into three age groups (under 40 years old, 41-59 years old, and over 60 years old), and the ABO blood type was distributed at each age No change between groups. Similarly, when men and women with COVID-19 were considered separately, the distribution of ABO blood types did not change much.

Zh
Discussion
This study found that the ABO blood group showed different associated risks for neocoronavirus infection. Specifically, blood group A is associated with increased risk, while blood group O is associated with decreased risk, thus proving that the ABO blood group is a biomarker of COVID-19 sensitivity difference.
These findings are consistent with other coronavirus infection risk patterns similar to ABO blood types found in previous studies. For example, previous studies have shown that the susceptibility of SARS-CoV infection in Hong Kong is related to the ABO blood group.
Researchers also found that hospital staff of blood group O were less likely to be infected than those of hospitals of non blood type O. Previously, anti-A antibodies were found to specifically inhibit the adhesion of SARS-CoV S protein-expressing cells to ACE2-expressing cell lines. In view of the similarity of the nucleic acid sequence between SARS-CoV and SARS-CoV-2 and the binding similarity of the receptor angiotensin-converting enzyme 2 (ACE2), the sensitivity of type O blood is low, while type A blood is less Higher sensitivity, which is related to the presence of natural anti-blood antibodies, especially anti-A antibodies, in the blood.
The research also mentions that this hypothesis will require direct research to prove. There may be other mechanisms for the susceptibility of ABO blood group to COVID-19, which needs further research to clarify.
Click to enter the topic:
Spotlight on new coronavirus pneumonia
Editor-in-chief: Yang Jie
Key words: ABO blood group AB blood group new coronary pneumonia Wuhan Hubei